|
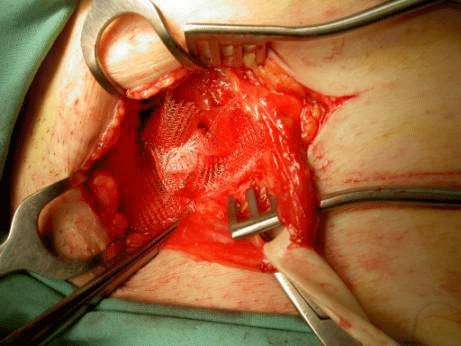
The use of mesh in hernia repair, risk management and the advantages of day surgery |
|||
Author:
Correspondence: Key words: day
surgery, hernia, mesh, local anaesthesia This
article has been prepared for primary care physicians. The introduction
is based on my experience with over 6000 hernia operations. It deals
with the history, examination, terminology, basic anatomy, pathology and
briefly the different surgical approaches. This is the first in a series
dealing with all the common hernias, their differential diagnosis and
then conditions of the scrotum and testis. In
Australia the patient must present to the GP to obtain a referral to a
specialist – otherwise the government health system will not cover the
cost of the consultation or surgical fees. The
doctor listens to the description of the onset of the symptoms – it
instills confidence into the patient and actually saves time. The
history can be important in making a positive diagnosis, and
differentiating between hernias and other conditions. Occasionally a
patient describes recurring swelling that cannot be demonstrated at the
time of examination. The presence of the hernia cannot be found at
examination, before careful and repeated evaluation. |
The
patient’s hernia region is then examined. The process should be
explained to the patient as palpation of the adjacent scrotal region can
cause embarrassment (this is part of risk management in Australia where
soaring indemnity payments has become an issue). The site is first inspected standing up at rest and then whilst coughing and straining. The hernia is usually apparent. During this process all possible sites for hernias should be inspected, including the opposite side for an inguinal or femoral hernia. It is surprising how often an additional femoral hernia or inguinal hernia can be detected in this manner. This avoids referring patients with an incomplete diagnosis. The hernia then may be palpated whilst standing. Then the hernia is palpated whilst the patient coughs and strains – looking for a cough impulse. Care must be taken not to hurt the patient by attempting to forcefully reduce an irreducible hernia. The
patient then lies down and is examined again. The
scrotal and testes region should also be examined whilst the patient is
standing and then recumbent. Some conditions are only detected whilst
the patient is standing. This includes a saphena varix, varicocele or
communicating hydrocoele. The
scrotal contents and the testes and other structures are palpated
carefully to exclude other conditions. The findings should be recorded
– especially any abnormality. The patient should be advised, for
example about the presence of a varicocele, so that following surgery it
is not thought to be a complication of surgery (risk management). |
||